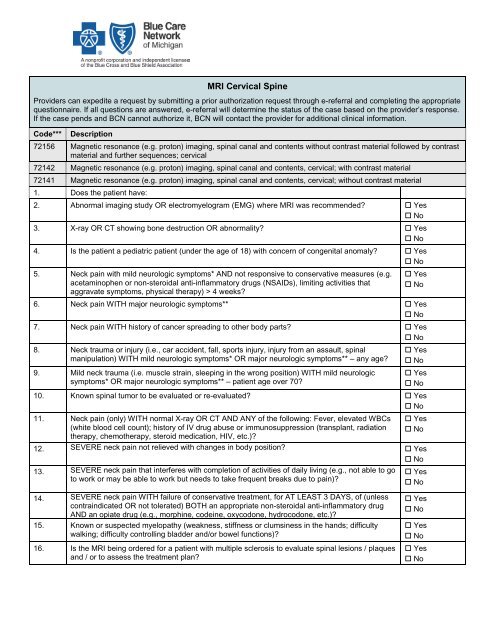
bcbs of michigan prior authorization form for radiology
|
Procedures that require authorization by eviCore healthcare
Authorization is required for all members for select outpatient cardiology interventional pain management radiation therapy radiology and physical |
|
Provider preauthorization and precertification requirements
23 jan 2024 · Providers can submit prior authorization requests for Blue Cross Blue Shield of Michigan radiology (high technology) and sleep studies (in lab) |
|
Procedures that require prior authorization by AIM Specialty Health
Overview Prior authorizations managed by AIM Specialty Health This document shows the codes associated with procedures that are managed by AIM for: |
|
Procedures that require prior authorization by AIM Specialty Health
Refer to the document Procedures that require authorization by eviCore healthcare Radiology (high technology) Blue Cross commercial Medicare Plus Blue BCN |
|
Procedures that require prior authorization by Carelon
To see the radiology procedures Carelon manages for those members refer to the document Procedures that require prior authorization by Carelon for Blue Cross |
Does CPT 93306 require authorization?
CPT 93306 — the procedure ordered most frequently by cardiologists via eviCore's Advanced Imaging and Cardiology program — will no longer require authorization effective January 1, 2023.
Is Blue Shield Michigan the same as Blue Cross Blue Shield?
Blue Cross Blue Shield of Michigan (BCBSM) is an independent licensee of Blue Cross Blue Shield Association.
|
BCBSM Request for Preauthorization Form
Blue Cross Blue Shield of Michigan Request for Preauthorization Form. Most preauthorization requests can be resolved by contacting Provider Relations and |
|
Provider Preauthorization & Precertification Requirements
Commercial Blue Cross Blue Shield of Michigan Products-Non-Medicare . Precertification request forms and instructions for submission are located at:. |
|
Provider Preauthorization and Precertification Requirements for
Jan 28 2022 Blue Cross Blue Shield of Michigan Definitions. • Prior Authorization. A process that allows physicians and other professional providers to ... |
|
Blue Cross and BCN: Procedures that require prior authorization by
Note: This list does not apply to Blue Cross and Blue Shield Federal Employee Program® Michigan members. To see the radiology procedures AIM manages for those |
|
BCN authorization requirements for non-Michigan providers
Mar 1 2022 For BCN commercial members |
|
Authorization requirements for Medicare Plus Blue PPO for
Jul 28 2022 For additional information |
|
Provider Preauthorization and Precertification Requirements for
5 days ago nursing long term acute care and rehab settings only. ? Assessment forms can be found at bcbsm.com/provider/quick-links.html. ? Do you still ... |
|
Blue Cross PPO Federal Employees Program Michigan members
Procedures that require prior authorization by AIM Specialty Health®. Radiology (high technology). For Blue Cross Blue Shield of Michigan on behalf of. |
|
Bcc-provider-manual.pdf
Jan 1 2019 Providers can access Blue Cross Complete forms at ... Provides coverage reviews for prior authorization after normal business hours. |
|
BCN referral and authorization requirements for Michigan providers
May 20 2021 the AAEC Evaluation Results Form and faxed to BCN. ... Authorization requests must be submitted prior to services being provided.Note: This. |
|
Provider Preauthorization & Precertification Requirements
Commercial Blue Cross Blue Shield of Michigan Products-Non-Medicare 2 Autism Spectrum Radiology Services 6 5/ 2018 Precertification request forms and instructions for submission are located at : |
|
Provider Preauthorization and Precertification - BCBSM
1 déc 2020 · for Blue Cross Blue Shield of Michigan PPO (commercial) and Medicare Medicare Plus Blue PPO Acute Fax Assessment form and submit the request via fax Refer to the Non-Michigan Provider Radiology Precertification, |
|
Bcbs of michigan prior authorization form - Squarespace
Bcbs of michigan prior authorization form Blue Cross Blue Shield of Michigan uses the following pre-certification and pre-authorization programs to ensure that |
|
Blue Cross Complete authorization requirements
30 sept 2020 · Providers should notify Blue Cross Complete of all emergency admissions Authorization request must be submitted at least 14 days prior to service Note: Coverage includes one set of X-rays of the spine per year Cross Complete Medication Prior Authorization Request form, which is available at |
|
Blue Cross Complete of Michigan authorization requirements
Services require authorization (This is a clarification of an existing requirement) using the Blue Cross Complete Medication Prior Authorization Request form, which is Note: Coverage includes one set of X-rays of the spine per year |
|
Authorization Requirements - Blue Cross Blue Shield
To obtain an authorization, Blue Cross Blue Shield of Prior authorization is required for out-of-network dialysis services only (Note: Authorization is not required for high-tech imaging provided as a component of an inpatient Management consent form and tentative treatment and discharge plan before admission; |
|
Prior Authorization of Physical Therapy and Occupational - eviCore
Prior Authorization of Physical Therapy and Occupational Therapy Blue Cross Blue Shield of Michigan Provider Orientation Blue Cross® Blue Shield® of |
|
PRIOR AUTHORIZATION REQUIREMENTS PPO - Health Net
PRIOR AUTHORIZATION REQUIREMENTS PPO (Self Funded and Fully Insured Plans) Home Depot Employees Implemented:01/01/2004 Prior Authorization |
|
Bcbsm - State of Michigan
Dear Subscriber: We are pleased you have selected Blue Cross Blue Shield of Michigan for your Therapeutic Radiology Diagnostic Radiology Prior Authorization Process "Waiver of Benefits” form acknowledging that the patient |
|
Welcome Provider Packet for BlueCross BlueShield of Michigan
BCBSM/BCN Medical Drug Authorizations Request Provider Welcome Packet Did you know that the form attached for the BCBSM – Medical Drug Prior Authorization link to be able to initiate MRI / CT scan / CPT codes / nursing codes )? |