bcbs of michigan prior authorization list
|
Provider preauthorization and precertification requirements
23 jan 2024 · Blue Cross Blue Shield of Michigan definitions • Prior authorization — A process that allows physicians and other professional providers |
|
State Health Plan Medicare Advantage Benefits
Prior authorization for certain services is key to making sure you receive Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent |
|
Prior Authorization Lookup Tool Available
30 oct 2020 · This new user-friendly resource allows users to enter a CPT or a HCPCS code to verify authorization requirements in real time before delivery |
|
Provider preauthorization and precertification requirements for Blue
Providers can submit prior authorization requests for Blue Cross Blue Shield of Michigan authorization requirements refer to the Carelon exclusion list for ... |
|
Blue Cross and BCN: Procedures that require prior authorization by
Note: This list does not apply to Blue Cross and Blue Shield Federal Employee Program® Michigan members. To see the radiology procedures Carelon manages for |
|
Blue Cross and BCN: Procedure codes for which providers must
For more information see the Services That Need Prior Authorization page on bcbsm.com. This document provides a detailed list of CPT* codes and HCPCS codes |
|
Blue Cross Blue Shield of Michigan Blue Care Network Prior
potential for off-label use and high-cost specialty drugs on this list require prior authorization for Blue Cross to cover them.. Questions? Please call the |
|
Blue Cross and BCN utilization management medical drug list
If “PPO” or. “HMO” appears in the Carelon column submit prior authorization requests to Carelon Medical Benefits Management (formerly known as AIM. Specialty |
|
BCN-managed procedure codes that require authorization for
6 дней назад Medical Drug and Step Therapy · Prior Authorization List for · Medicare ... musculoskeletal surgical and related procedures for Blue Cross Blue ... |
|
Preferred Drug List Prior Authorization and Step Therapy Coverage
Blue Cross Blue Shield of Michigan and Blue Care Network work to make sure you get the safest most effective and most reasonably priced prescription drugs. Our |
|
Blue Cross and BCN: Determining prior authorization requirements
22 февр. 2023 г. Provider's location. Situation. Michigan. I need to look up requirements for a member who has: • Coverage through Blue Cross Blue Shield of ... |
|
Your 2023 Blue Cross Shield of Michigan Clinical Drug List
Additional coverage requirements may apply for preferred alternatives such as prior authorization. Specialty drugs. For more information on specialty drugs |
|
Blue Cross and BCN: Musculoskeletal procedure codes that require
(2)This procedure code doesn't require prior authorization for Blue Cross commercial members. Blue Cross Blue Shield of Michigan and Blue Care. Network. |
|
Provider Preauthorization and Precertification Requirements for
28 janv. 2022 Blue Cross Blue Shield of Michigan precertification services are available 24 ... For an up-to-date list of states and effective dates ... |
|
Blue Cross and BCN: Procedures that require prior authorization by
Note: This list does not apply to Blue Cross and Blue Shield Federal Employee Program® Michigan members. To see the radiology procedures AIM manages for those |
|
Provider Preauthorization and Precertification Requirements for
4 août 2022 providers can be reviewed on the BCBSM Mental Health Carve-Out List. Call New Directions at 800-762-2382 to obtain precertification and ... |
|
Provider Preauthorization & Precertification Requirements
Behavioral Health. Commercial Blue Cross Blue Shield of Michigan Products-Non-Medicare. Precertification is required for: • Psychiatric inpatient admissions. |
|
BCBSM & BCM Prior Authorization and Step Therapy coverage criteria
1 sept. 2022 potential for off-label use and high-cost specialty drugs on this list require prior authorization for Blue Cross to cover them.. Questions? |
|
Blue Cross and BCN utilization management medical drug list
Pharmacy Services page on our bcbsm.com website. See the Medical oncology prior authorization list for Blue Cross and BCN commercial members for a. |
|
Blue Cross Blue Shield of Michigan Blue Care Network - Preferred
1 sept. 2022 Blue Cross Blue Shield of Michigan. Blue Care Network. Preferred Drug List. Prior Authorization and Step Therapy Coverage Criteria. |
|
BCN authorization requirements for non-Michigan providers
1 mars 2022 Providers contracted with a Blue Cross Blue Shield plan must request prior authorization for the services listed in the table below. |
|
Medical Drug and Step Therapy Prior Authorization List for Medicare
4 oct. 2021 Medical Drug and Step Therapy Prior Authorization List ... authorizations of select services for Blue Cross Blue Shield of Michigan and Blue. |
|
Utilization Management Program Quick Reference Guide
is an independent company that manages prior authorization for Blue Cross Blue Shield of Michigan. ... Authorization is required for Medicare Plus Blue. |
|
Provider Preauthorization and Precertification - BCBSM
1 déc 2020 · Provider Preauthorization and Precertification Requirements for Blue Cross Blue Shield of Michigan PPO (commercial) and Medicare Plus |
|
Provider Preauthorization & Precertification Requirements
Provider Preauthorization Precertification Requirements Table of Commercial Blue Cross Blue Shield of Michigan Products-Non-Medicare Before calling, providers should view the Hospitals and Facilities List of Benefits ( PDF) |
|
Michigan Prior Authorization Request Form for Prescription Drugs
Prior authorization requests are defined as requests for pre-approval from an insurer for □Priority □Magellan □Blue Cross Blue Shield of Michigan □HAP □ |
|
Blue Cross and BCN procedures that require authorization - eviCore
Go directly to the BCN code lists Overview Select Blue Cross Blue Shield of Michigan PPO (commercial) and Blue Cross Medicare Plus Blue Providers must obtain authorization from eviCore before these services are provided |
|
Prior Authorization of Outpatient Physical Therapy and - eviCore
Blue Cross Blue Shield of Michigan and Blue Care Network are nonprofit corporations and independent licensees eviCore is an independent company that manages prior authorization for List of CPT codes that require prior authorization |
|
Bcbs of michigan prior authorization form - Squarespace
Blue Cross Blue Shield of Michigan uses the following pre-certification and 2016 The Medicare Plus Blue (PDF) Pre-Authorization Code List represents |
|
Blue Cross Complete authorization requirements
30 sept 2020 · Providers should notify Blue Cross Complete of all emergency Authorization request must be submitted at least 14 days prior to service Please click this link to view a list of genetic testing codes that require authorization |
|
Blue Cross Blue Shield of Michigan and Blue Care Network Updates
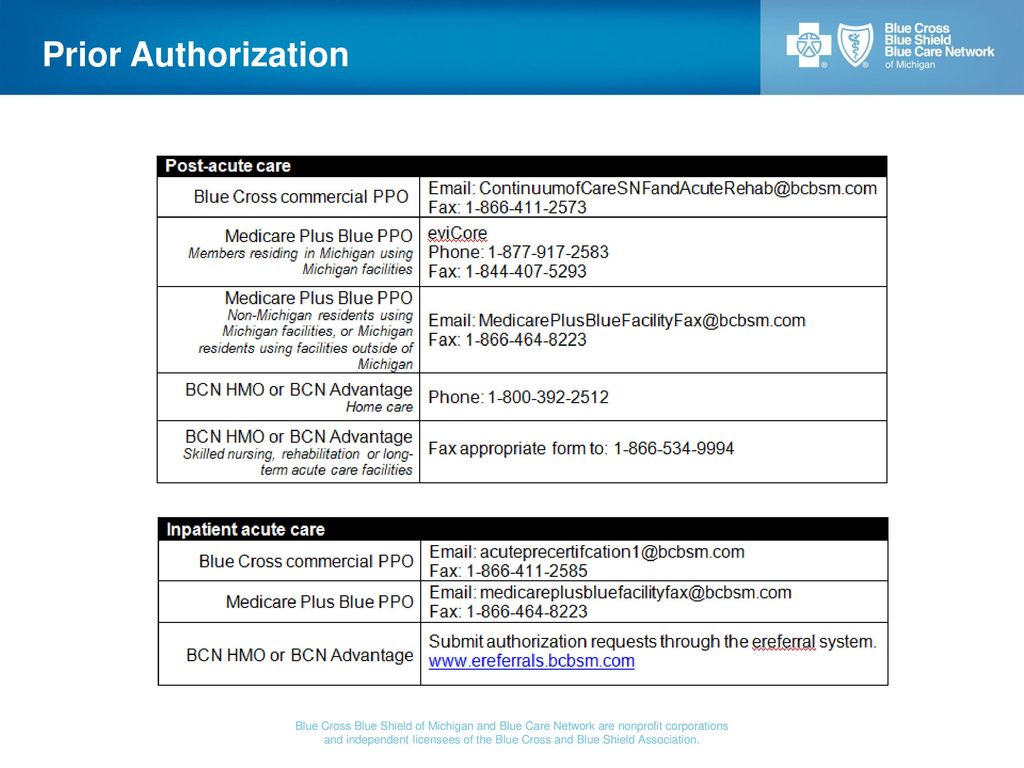
3 nov 2017 · Prior authorization contact list for Blue Cross commercial PPO, Medicare Plus BlueSM, BCN HMOSM, BCN AdvantageSM Blue Cross Blue |
|
Blue Cross Blue Shield of Michigan - MSU HR - Michigan State
BCBSM's prior authorization process Request for Drugs Not on BCBSM's Drug List coverage of a prescription drug not on the list before it is dispensed |
|
BCBSM/BCN Custom Drug List
BCBSM and BCN Custom Drug List (Formulary) introduction 5 Blue Care Network Prior authorization and step therapy guidelines 8 Blue Cross Blue Shield of |