antibiotic resistant sinus infection
|
Stanford Antimicrobial Safety and Sustainability Program 12
Considerations: Most (90-98 ) cases of acute rhinosinusitis are due to a viral infection that will self-resolve In most cases symptoms improve within two weeks regardless of whether they receive an antibiotic or not 1 Patients that are significantly Immunocompromised or have chronic or recurrent (4 or more episodes per year) sinusitis may |
|
AAO-HNSF Updated Clinical Practice Guideline: Adult Sinusitis
Choice of Antibiotic for Acute Bacterial Rhinosinusitis (ABRS) antibiotic agent the clinician should 10 days for most adults – If a decision is made to treat ABRS with an prescribe amoxicillin with or without clavulanate as first-line therapy for 5 to – If the patient fails to improve with the initial 6 |
|
Adult Acute Bacterial Rhinosinusitis (ABRS) Guideline
No Risks for Antibiotic Resistance Present ymptoms for ABR Present Assess risk factors for antibiotic resistance: •Use of antibi ti c swit hin t epre eding 4 eeks • Hospitalization within the past 5 days • Severe co-morbidities Assess Adult Patient for Acute Rhinosinusitis Provide supportive care (TABLE A) plus an antibiotic*: |
When do I really need antibiotics for a sinus infection?
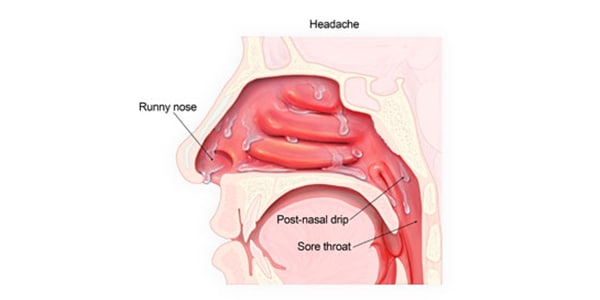
When do sinus infections need antibiotic treatment? Antibiotics may be needed when a secondary bacterial infection accompanies the primary viral infection. A clear sign of this will be high fever (>100 degrees) and facial pain that persists for more than five days.
When do you really need antibiotics for that sinus infection?
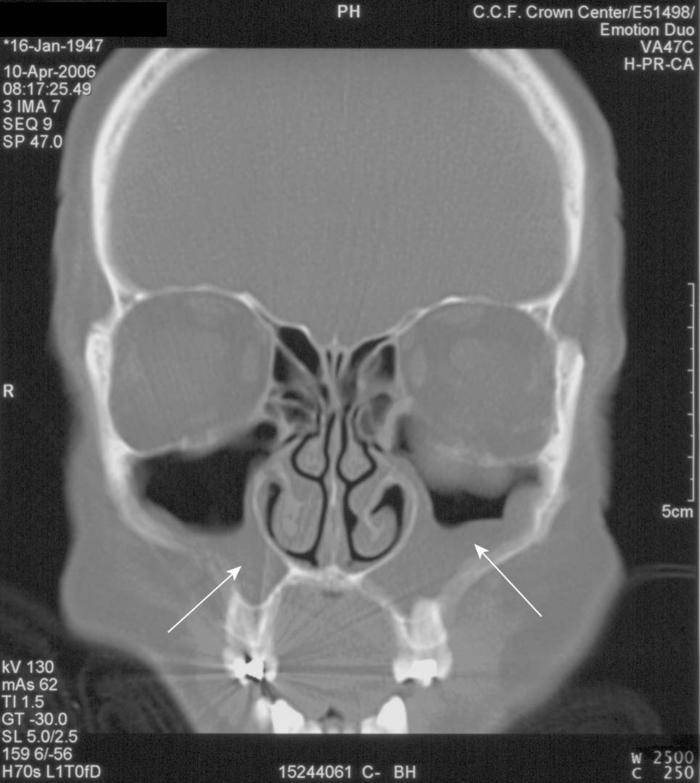
X-rays cannot tell if the infection is due to a virus or bacteria, so are not particularly helpful. Antibiotics should be reserved for patients whose symptoms persist for over 10 days, are severe, or deteriorate after initial improvement. Severe symptoms include fever over 102, discolored nasal drainage, facial pain for over 3 days.
What is the best antibiotic to treat a sinus infection?
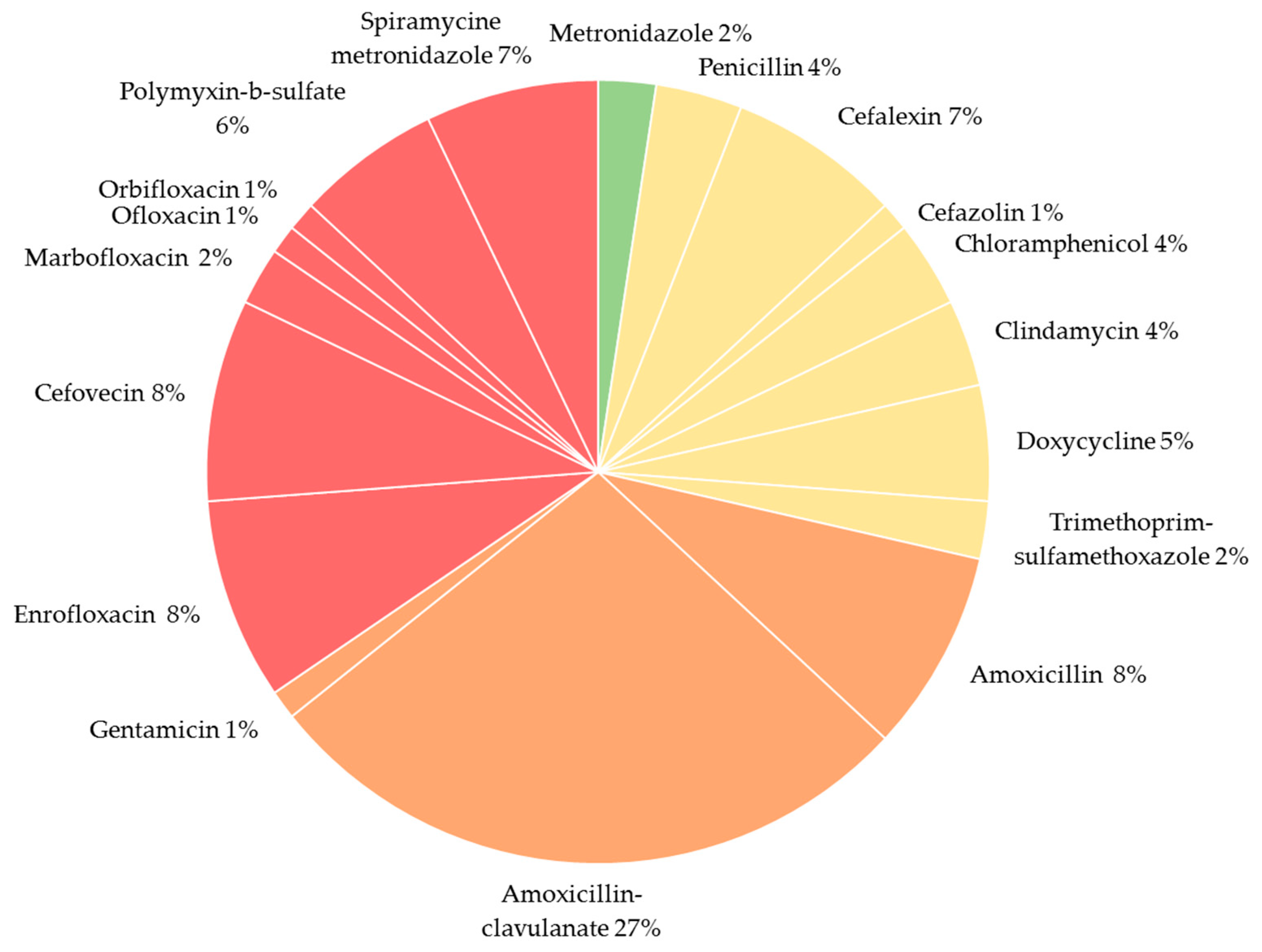
Treatment of Chronic Sinusitis The antibiotics of choice include agents that cover organisms causing acute sinusitis but also cover Staphylococcus species and anaerobes. These include amoxicillin-clavulanate, cefpodoxime proxetil, cefuroxime, gatifloxacin, moxifloxacin, and levofloxacin.
Do sinus infections respond well to antibiotics?
This means that the majority of the time, antibiotics are unnecessarily prescribed. Of all sinus infections, 85% clear up on their own, while only 15% do not. This 15% is the population that needs antibiotics. Consuming antibiotics, even when you need them, increases side effects and bacterial resistance rates.
|
Antibiotics Arent Always the Answer: CDC
More than 2.8 million antibiotic-resistant infections occur in the United Sinus infection. Maybe. Middle ear infection. Maybe. Bronchitis/chest cold (in ... |
|
Assessing the health burden of infections with antibiotic-resistant
Suggested citation: European Centre for Disease Prevention and Control. Assessing the health burden of infections with antibiotic-resistant bacteria in the EU/ |
|
Cdc
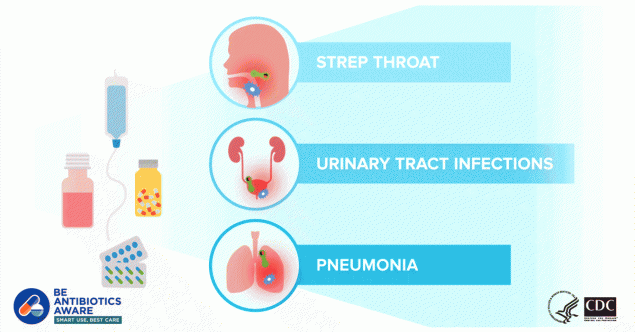
It also is a major cause of bloodstream infections and ear and sinus infections. RESISTANCE OF CONCERN. S. pneumoniae has developed resistance to drugs in |
|
Cdc
It also is a common cause of bloodstream infections and ear and sinus infections. WHAT YOU NEED TO KNOW. □ Overall |
|
2022 SPECIAL REPORT: COVID-19 U.S. Impact on Antimicrobial
12 июл. 2022 г. In 2020 14% of Salmonella infections were resistant to at least one antibiotic used to treat severe infection. ... nasal) were excluded. Among ... |
|
Antibiotics Arent Always the Answer (CDC)
More than 2.8 million antibiotic-resistant Antibiotics also won't help some common bacterial infections including most cases of bronchitis |
|
Antibiotic Use in the United States 2018 Update: Progress and
antibiotics are needed for sinus infections. “Uncomplicated” means that the patient: □ is at low risk of developing an antibiotic-resistant infection. |
|
Antibiotic Use in the United States 2017: Progress and Opportunities
that do not always need antibiotics (like many sinus and ear infections). difficile infection and antibiotic-resistant infections. This is especially ... |
|
World Health Day: Media Fact Sheet
7 апр. 2011 г. outpatient settings drives antibiotic resistance and increases one's chance of acquiring an antimicrobial-resistant infection. Therefore it ... |
|
Treating Sinus Infections: Dont rush to antibiotics
Overuse of antibiotics also promotes the growth of bacteria that can't be controlled easily with drugs. That makes you more vulnerable to antibiotic-resistant |
|
Antibiotic Resistance Threats in the United States 2019 (2019 AR
13 nov. 2019 More than 2.8 million antibiotic-resistant infections occur in the United ... cause of bloodstream infections and ear and sinus infections. |
|
Antibiotic Resistance Threats in the United States 2013
23 avr. 2013 CDC's Work to Prevent Infections and Antibiotic Resistance in Healthcare ... cause of bloodstream infections and ear and sinus infections. |
|
Treating Sinus Infections: Dont rush to antibiotics
Overuse of antibiotics also promotes the growth of bacteria that can't be controlled easily with drugs. That makes you more vulnerable to antibiotic-resistant |
|
Antibiothérapie par voie générale en pratique courante dans les
30 déc. 2003 dans les infections ORL néanmoins l'évolution de sa résistance est ... Les bactéries prolifèrent dans les sinus réalisant une sinusite ... |
|
Antibiotic Use in the United States 2018 Update: Progress and
antibiotics are needed for sinus infections. “Uncomplicated” means that the patient: ? is at low risk of developing an antibiotic-resistant infection. |
|
Antibiotic Use in Outpatient Settings
such as sinus infections middle ear infections |
|
ANTIBIOTICS ARENT ALWAYS THE ANSWER
including most cases of bronchitis many sinus infections |
|
Drug-Resistant Streptococcus pneumoniae
It also is a common cause of bloodstream infections and ear and sinus infections. Rates of antibiotic-resistant invasive pneumococcal infections. |
|
Azithromycin: An Underappreciated Quinolone-Sparing Oral
13 avr. 2022 sinusitis; skin infection; otitis media. 1. Introduction. The rapid spread of antibiotic resistance and high treatment failures in Gram- ... |
|
ANTIBIOTICS ARENT ALWAYS THE ANSWER Fact Sheet
including most cases of bronchitis many sinus infections |
|
Sinusitis and antibiotics - The Lancet
12 mai 2012 · antibiotics leads to emergence of antibiotic-resistant bacteria Thus nasal discharge after a viral upper respiratory infection of 5–6 days that |
|
Treating Sinus Infections: Dont rush to antibiotics - Choosing Wisely
Overuse of antibiotics also promotes the growth of bacteria that can't be controlled easily with drugs That makes you more vulnerable to antibiotic- resistant |
|
IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in
Furthermore, treatment failure was associated with the recovery of antibiotic- resistant pathogens [29] However, sinus aspiration is an invasive, time- consuming, |
|
Antibiotics Mostly Useless for Sinusitis - University at Buffalo
20 déc 2006 · 18 (HealthDay News) -- If you develop a mild sinus infection this winter -- or become colonized with antibiotic-resistant bacteria such as S |
|
Clinical trial of the treatment of acute sinusitis - Clinical Trialsgov
risk of penicillin-resistant S pneumonia in the community is greater than 10 sinuses are likely--for some antibiotics, and in particular for amoxicillin--to be |
|
Role of antibiotics in sinusitis - Infectious Disease and Antimicrobial
Sinusitis is a leading reason for outpatient antibiotic use, but symptoms are A bacterial sinus infection bacterial sinusitis depend on the resistance patterns |
|
Choosing an Antibiotic for Sinus Infection, Otitis Media - PCORI
Broad-Spectrum Antibiotics for Common Infections in Children sinusitis—make decisions with parents about the medicine that is best for the child The study the likelihood of antibiotic resistance, which may limit the use of these medicines |
|
The diagnosis and management of sinusitis: A practice - AAAAI
For chronic infectious sinusitis, a longer sinusitis and unnecessary treatment with antibiotics Ap- Medically resistant sinusitis might respond to appro- |