bcbs denial codes list
|
Blue Cross Complete of Michigan
Blue Cross Complete of Michigan New and Current Explanation of Benefit (EOB) Codes - Effective August 1 2020 EOB Code EOB Description Claim Adjustment Reason Code Claim Adjustment Reason Code Definition Remittance Remark Code Remittance Adjustment Reason Code Definition Provider Adjustment Reason Code |
|
BCBSTX Ineligible Reason Code List
1 INELIGIBLE REASON CODE LIST CATEGORY INELIGIBLE REASON CODE PROVIDER CLAIM SUMMARY MESSAGE PRE-PAY REVIEW AP1 ADDITIONAL INFORMATION IS REQUESTED FROM THE PROVIDER IF NO RESPONSE IS RECEIVED WITHIN 45 DAYS OF THIS NOTICE NO FURTHER NOTICE WILL BE GIVEN AND BENEFITS WILL BE CONSIDERED DENIED PRE-PAY REVIEW AP2 |
What are Blue Cross Blue Shield denial codes?
Blue Cross Blue Shield denial codes or Commercial insurance denials codes list is prepared for the help of executives who are working in denials and AR follow-up.
What is a health care denial code?
Denial codes are alphanumeric codes assigned by insurance companies to communicate the reasons for rejecting or denying a health care claim submitted by a medical provider. These codes help you understand the specific issues that led to the denial, allowing you to take appropriate actions to rectify them and resubmit the claim.
Why is my claim denied with code CO 11?
Payers deny your claim with code CO 11 when the diagnosis code you submitted on the claim doesn’t align with the procedure or service performed. This situation can arise for several reasons, such as: Making a typo in the diagnosis code. Using an incorrect diagnosis code.
What are the requirements for a bcbsms occurrence code 25 claim?
The records at BCBSMS indicate that this should be a secondary claim which requires primary insurance information to be provided on the claim. Inpatient claim must have an attending physician NPI Inpatient claim must have an attending physician first and last name. If occurrence code 25 is present, non-covered charges must equal total charges.
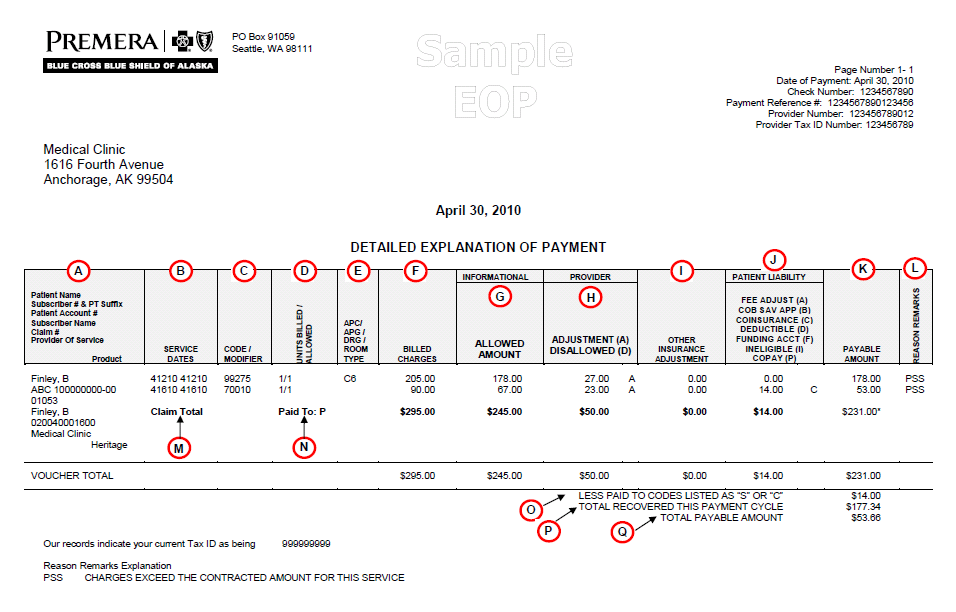
Where Are Denial Codes located?
You can find denial codes on electronic remittance advice. It includes details about claim processing, covering payment or denial information. We’ve highlighted some codes that you can find in electronic remittance advice below. selecthub.com
Reason For Denials
Understanding the reasons for denials is essential, as it enables you to address and rectify issues, ensuring a smoother and more efficient revenue flow while providing patients with the care they need. We’ve highlighted some of the reasons below. selecthub.com
How to Avoid Denials
Denials can damage the financial health of your practice or company. Now that you know the common reasons and denial codes, you can predict and prevent denials. We’ve highlighted some ways to help you avoid denials below. selecthub.com
FAQs
How can I file an appeal? You can file for an internal appeal or external review. Follow the steps below to file an internal appeal. 1. Write a letter to the insurance company requesting an internal appeal. You should include the patient’s name, claim number and health insurance ID. 2. Attach the explanation of benefits to the letter to show denied services. 3. Send supporting documents and a letter to the insurance provider. Remember you need to file an internal appeal within 180 days after you receive a denial. If i
Next Steps
Handling denials is daunting. Insurance companies might deny your claim for minor discrepancies, causing revenue losses. Medical billing software can save you from making silly mistakes and help you submit clean claims. But how do you compare hundreds of products quickly? Don’t worry We got you covered You can refer to our free comparison reportt
Related Articles
Best Medical Compliance Software for PracticesKey Steps to Follow for a Successful Medical Billing ProcessBest Free Medical Billing Software selecthub.com
|
BCBSTX Ineligible Reason Code List
CLAIM PAYMENT HAS BEEN REDUCED DUE TO LATE PREAUTHORIZATION AS REQUIRED BY. YOUR BLUE CROSS BLUE SHIELD OF OKLAHOMA PARTICIPATING PROVIDER CONTRACT. |
|
New and Current Explanation of Benefit (EOB) Codes
EOB codes begin with an upper case alpha value. This list includes new and current EOB codes. Page 1 of 55. Page 2. Blue Cross Complete of Michigan. New and ... |
|
Claim Denial Codes List
Remittance Advice Remark Code (RARC). Description. Medicaid. Error Code CLAIM DENIAL CODES LIST as of 08/14/2023. Page 2. 1847. Invalid place of service. 2083. |
|
Blue Cross and BCN: Appealing a clinical editing denials - instructions
You should submit the documentation appropriate to the procedure code that was denied and the denial reason. Take other considerations into account: Blue Cross |
|
ANSI-reason-codes.pdf
Although reason codes and CMS message codes will appear in the body of the remittance notice the text of each code that is used will be printed at the end of |
|
Claim Adjustment Reason Codes (CARC)
CARC CODE DESCRIPTION. 1. Deductible Amount. 2. Coinsurance Amount. 3. Co-payment Amount. 4. The procedure code is inconsistent with the modifier used. |
|
Claim Status Tool User Guide
Feb 1 2023 ... list. Enter the Member ID including the preceding three-character ... Note: Additional Action(s) only display for certain ineligible reason codes. |
|
Claims Error Manual for
If the procedure code falls in the DSP list then the NDC must be present E-code cannot be reason for visit. UB0269. Invalid procedure code (grouper). UB0270. |
|
EOB Code Description Rejection Code Group Code Reason Code
Remark. Code. 122 History adjustment due to consolidation of claim numbers list all claims in Box 11. Electronic Billers use remarks. Dept. will split ... |
|
Claim Status Tool User Guide
list or enter the Provider NPI (Type 2). Enter the Member ID includingthe ... → Ineligible reason codes display in the Codes field. → View ineligible ... |
|
New and Current Explanation of Benefit (EOB) Codes
Non-covered Service list. 96. Non-covered charge(s). At least one Remark Code must be provided (may be comprised of either the NCPDP Reject Reason Code |
|
ANSI-reason-codes.pdf
Although reason codes and CMS message codes will appear in the body of the remittance notice the text of each code that is used will be printed at the end of |
|
Claim Denial Codes List
Claim Denial Codes List as of 03/01/2021. Claim Adjustment Reason Code (CARC). Remittance Advice Remark Code (RARC). Medicaid Denial Reason. |
|
ADJUSTMENT REASON CODES REASON CODE DESCRIPTION 1
must be provided (may be comprised of either the Remittance Advice Remark Code or NCPDP Reject. Reason Code.) 18. Duplicate claim/service. |
|
Appendix A
This table contains the Health Care Claims Adjustment Reason Codes For current code lists |
|
Crosswalk - Adjustment Reason Codes and Remittance Advice (RA
Code or RA Remark Code is listed once. Example #1: EX of 10 and 1e - EX 10 translates to 42 and N14 and EX 1e translates to 42 and MA23. The RA would list |
|
EOB Code Description Rejection Code Group Code Reason Code
Code. Remark. Code. 001 Denied. Care beyond first 20 visits or 60 days requires 065 Only one adjustment form should be submitted listing all. |
|
Blue Cross / BCN Clinical Editing Appeal Form
Click here re. accessing the BCN codes list. Blue Cross commercial. Use this form only when appealing a clinical editing denial decision for PPO EOP codes. |
|
HIPAA Claims Adjustment Reason Codes - Facets (last updated 29
NCPDP Reject Reason Code or Remittance Advice Remark. Code that is not an ALERT. This edit occurred because the Revenue Code is not in Medicare's list. |
|
Provider Remittance Advice Codes - Alabama
Explanation of Benefit (EOB) Claim Adjustment Reason Codes (CARC) and Remittance Advice Remark Codes (RARC) may appear on a. Provider Remittance Advice |
|
Commercial Remittance Advice Code Descriptions - Blue Cross
31 jan 2018 · adjustment reason and remark codes can be accessed on the Washington Publishing For a list of eligible maternity codes see BCBST com |
|
Appendix A: Health Care Claims Adjustment - Blue Cross NC
This table contains the Health Care Claims Adjustment Reason Codes, For current code lists, access the Washington Publishing Web site at http://www wpc- |
|
Blue Cross Complete explanation of benefit codes
least one Remark Code must be provided (may be comprised of either the NCPDP Reject Reason This list includes new and current EOB codes Page 1 of 55 |
|
EOB Code Description Rejection Code Group Code Reason - L&I
Remark Code 040 Denied Place of service is invalid/invalid for date of service Resubmit 232 You must list all applicable modifiers in remarks when billing |
|
Claim Adjustment Reason Codes - NDgov
At least one Remark Code must be provided (may be comprised of either the NCPDP Reject Reason Code, or Remittance Advice Remark Code that is not an |
|
ANSI REASON CODES
Although reason codes and CMS message codes will appear in the body of the remittance notice, the text of each code that is used will be printed at the end of the |
|
Adjustment Reason Codes and Remittance Advice - Partnership
Code or RA Remark Code is listed once Example #1: EX of 10 and 1e - EX 10 translates to 42 and N14 and EX 1e translates to 42 and MA23 The RA would list |
|
Anthem Blue Cross and Blue Shield Provider and Facility Manual
Blue Cross and Blue Shield names and symbols are registered marks of the Blue Cross and Blue Shield Association Directory of Services/Provider Resource Information This Manual includes CPT codes selected by Anthem No fee encounter and claim data to HHS for purposes of risk adjustment Because HHS |
|
How to correct rejected claims - Provider Central - Blue Cross Blue
HIPAA standard adjustment reason code narrative: The benefits for this service are included in the payment/allowance for another service/procedure that has |