bcbs payer id
|
Payer ID provider number reference — Professional
Payer ID provider number reference — Professional Use this guide as a reference tool when submitting professional claims The information was current at the time of publication We will announce changes on the Provider News Center and the Provider Engagement Analytics & Reporting (PEAR) portal and Blue Shield Association |
How do I submit a Blue Cross & Blue Shield claim?
Download and complete the appropriate form below, then submit it by December 31 of the year following the year that you received service. (For example, if your service was provided on March 5, 2022, you have until December 31, 2023 to submit your claim). If you have questions, please contact your local Blue Cross and Blue Shield company.
What is a payer ID & EDI lookup tool?
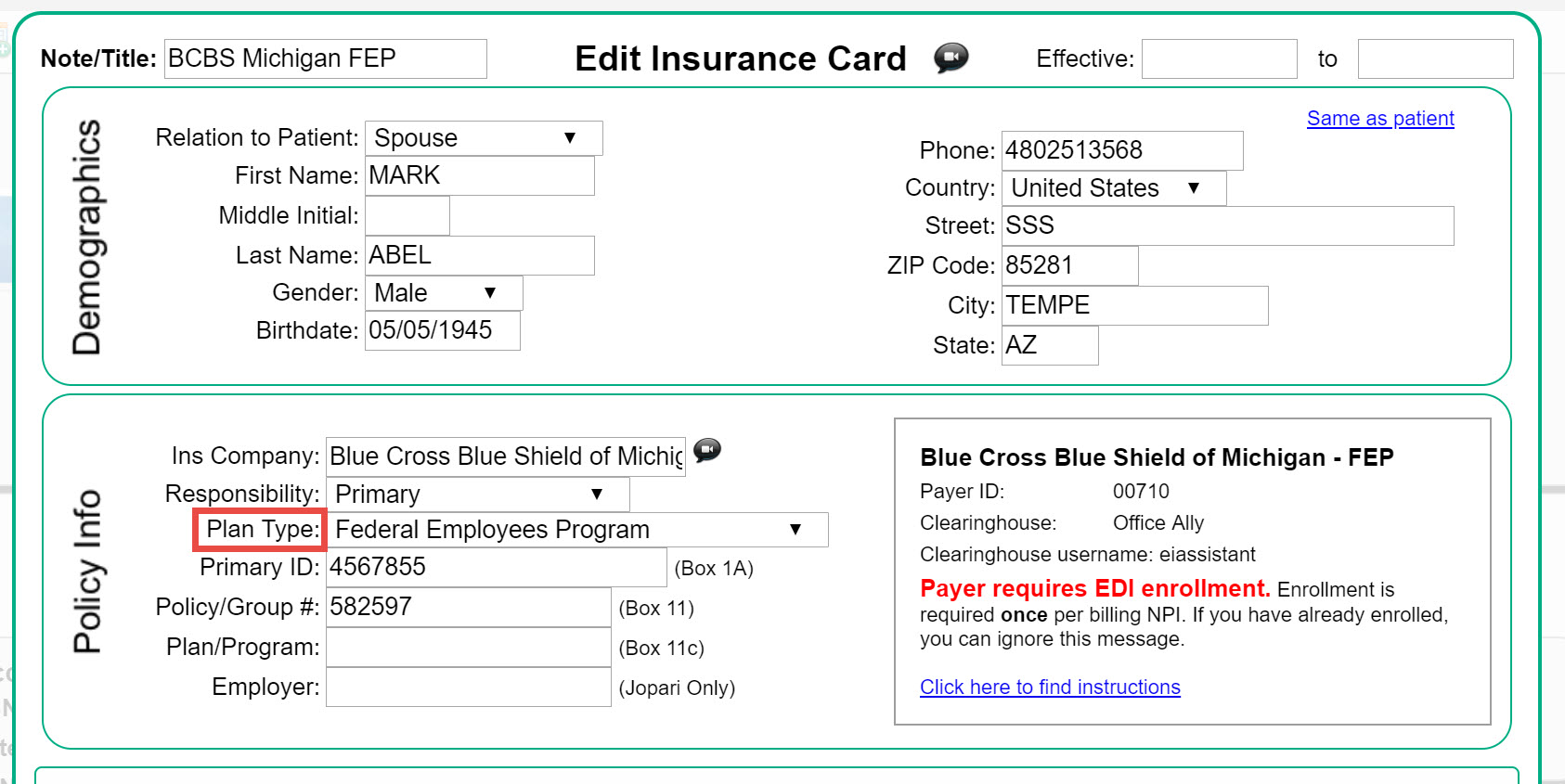
Below I have shared all the information which you need to know about payer IDs along with payer id lookup tool. What is Payer ID on insurance card? Payer ID (also known as payor ID OR EDI) is a unique ID assigned to each insurance company e.g. Cigna, BCBS, United Healthcare to receive claims electronically.
What is a payer ID?
A Payer ID routes electronic data transactions to the appropriate payer. Healthcare Eligibility Benefit Inquiry and Response (270/271) Healthcare Services Inpatient Admission and Discharge Notification (278N) To send claims via the Availity EDI Gateway, log in to the Availity site. Don't have an Availity account?
Do I need a different payer ID if I transmit through a clearinghouse?
If you transmit through a clearinghouse, the clearinghouse may require different payer IDs. *PAI and Blue Solutions Administrators are separate companies that provide third party administration services on behalf of BlueCross. BlueChoice HealthPlan is an independent licensee of the Blue Cross and Blue Shield Association.
|
Blue Cross Blue Shield of Michigan Electronic Interchange Group
Nov 18 2021 Blue Cross Blue Shield of Michigan |
|
Payer-id-provider-number-reference-professional.pdf
When treating non-Independence members professional providers who are contracted with other local area. Blue Cross and/or Blue Shield. (BCBS) health plans ( |
|
Update Minnesota Health Care Programs Payer ID
Jan 23 2019 Claims for Blue Cross and Blue Shield of Minnesota and Blue Plus Minnesota Health Care Programs (MHCP) subscribers |
|
Quick tips to filing a complete and correct professional claim
Feb 21 2022 Anthem Blue Cross and Blue Cross of California Partnership P lan |
|
Payer-id-provider-number-reference-facility.pdf
Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan Keystone Health Plan East |
|
New Payer ID for Blue Cross Medicare Advantage
Jan 1 2017 New Payer ID o The Payer ID for the Blue Cross Medicare Advantage plans will change to 66006 for claims submitted on and after Jan. 1 |
|
Payer ID Tech ID OI Code Coverage Type Payer Phone Street City
PO BOX 2500/600. LAFAYETTE. DETROIT. MI. MEDCO BCBS. 00038005. 359274. 89. X3. (800) 482-3600 600 LAFAYETTE. DETROIT. MI. BC BS FEDERAL EMPLOYEE PROGRAM. |
|
How to Locate the Payer ID (EDI)
The Payer ID or EDI is a unique ID assigned to each insurance company. It allows provider and payer systems to talk to one another to verify eligibility |
|
Blue Cross Community Options SM – Electronic Claim Submission
Nov 1 2015 Payer ID – MCDIL. On Dec. 9 |
|
New Payer ID for Blue Cross Medicare Advantage
Jan 1 2017 New Payer ID o The Payer ID for the Blue Cross Medicare Advantage plans will change to 66006 for claims submitted on and after Jan. 1 |
|
Commercial Payer Listing - Blue Cross Blue Shield of Michigan
23 déc 2020 · Blue Cross Blue Shield of Michigan, Electronic Interchange Group Professional Commercial Payer List Payer ID Claim Office # Type Name |
|
Payer ID provider number reference - Independence Blue Cross
independent licensees of the Blue Cross and Blue Shield Association Look for announcements about revised payer ID grids in Partners in Health UpdateSM |
|
EDI Payer ID List - Highmark Blue Shield
EDI Payer ID List 93688 AmeriHealth – Delaware – Non HMO 60061 AmeriHealth – New Jersey - Non HMO 54763 AmeriHealth Administrators 60147 First |
|
Payer Specification Sheet - Prime Therapeutics
1 jan 2020 · Payer Requirement: Required for BCBS of RI Work Related Injury only, BIN 61Ш455, PCN BCRI Required for Capital Blue Cross BIN |
|
Claims and Remits Payer List - Experian
12 mar 2021 · Payer 75185 to HealthSmart Benefit Solutions (EDI Payer ID Anthem Blue Cross Blue Shield of California (Claims and Encounters) 47198 |
|
Medicare Secondary Payer - Blue Cross Blue Shield
The Centers for Medicare Medicaid (CMS) has rules for determining when other types of insurance such as an employer's group health plan must pay primary |
|
Filing Claims- Electronic Filing - HMO Provider Manual - Blue Cross
Blue Cross and Blue Shield of Texas (BCBSTX) supplies Payer Response Reports to our Electronic Data Interchange (EDI) Partners from the BCBS claims |
|
Plan Name Member ID Prefix Payer ID BlueCross BlueShield of
Payer ID BlueCross BlueShield of South Carolina Preferred BlueSM and BlueEssentialsSM (also includes all out‐of‐state BlueCard members) All prefixes |
|
WATCHMAN Payer List
26 REIMBURSEMENT GUIDE WATCHMAN Private Payer Coverage (January 2021) BCBS of Federal Employee Program National AvMed FL Blue Cross |
|
Blue Cross Complete Claims Filing Instructions
1 oct 2020 · Verification of whether there is Medicare coverage or any other third party resources and, if so, verification that the Plan is the “payer of last resort” |