calchoice cobra forms
| Important COBRA and Cal-COBRA Information |
How do I request a Cal-Cobra extension?
Beneficiary must contact Cal-COBRA ( 800-228-9476) to request the extension and ensure they meet the requirements. If approved, the beneficiary will submit this form to formally accept the extension. Once the employer submits the ENF (C13140), an Election packet is sent to the beneficiary.
What is Cal-Cobra & how does it work?
Cal-COBRA is a California Law that lets you keep your group health plan when your job ends or your hours are cut. It may also be available to people who have exhausted their Federal COBRA. Cal-COBRA applies to employers and group health plans that cover from 2 to 19 employees. Federal COBRA — 18 or 36 months.
Does Cal-Cobra apply to individual health insurance?
Cal-COBRA does not apply to individual health insurance. As of January 1, 2003, the extension period for Cal-COBRA has been changed from 18 months to 36 months. If you become eligible for Cal-COBRA after January 1, 2003, you will have the benefit of Cal-COBRA coverage for a full 36 months instead of the prior 18-month coverage extension.
What is a cobra form?
COBRA Forms. If you are an employee of the Commonwealth of Massachusetts, you have the right to choose COBRA coverage if you lose your group health coverage because your hours of employment are reduced or your employment ends for reasons other than gross misconduct.
|
EMPLOYER ADMINISTRATIVE GUIDE
Domestic Partner Eligibility Under COBRA . Employer Responsibilities For Cal-COBRA . ... Preference Form also found on our website calchoice.com. |
|
MyCalchoice
Employer Responsibilities For Cal-COBRA . Language Assistance Preference Form also found on our website www.calchoice.com. www.calchoice.com ... |
|
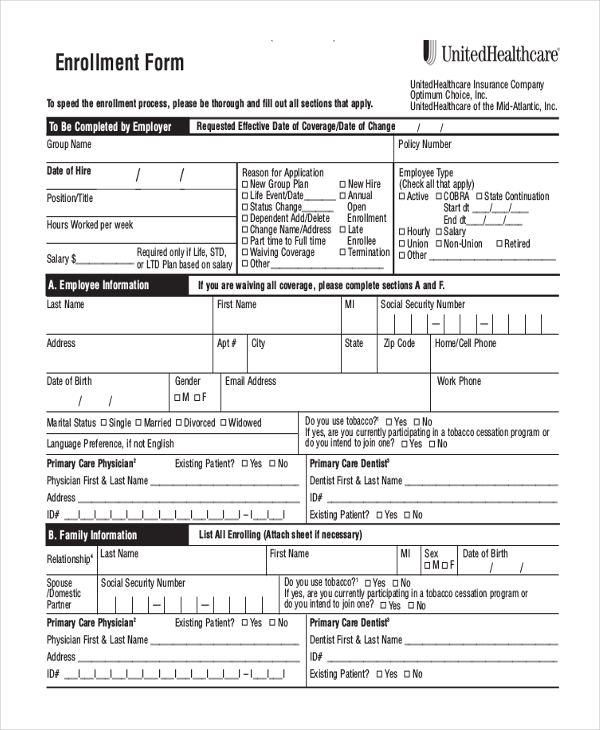
Member enrollment guide
COMPLETE AN EMPLOYEE CHANGE REQUEST FORM IF YOU ARE AN EXISTING MEMBER AND NEED TO MAKE CHANGES. www calchoice com Just click on “Rx Search” in the top. |
|
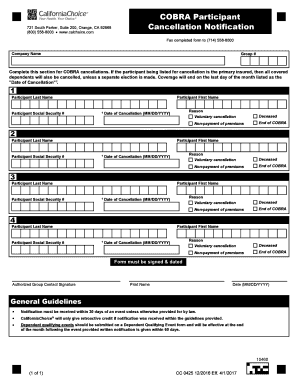
COBRA Enrollment Application
EMPLOYER: Complete section below - then provide form to COBRA eligibles for completion. COBRA Enrollment Application (800) 558-8003 www.calchoice.com. |
|
EMPLOYER ADMINISTRATIVE GUIDE
Domestic Partner Eligibility Under Cal-COBRA . Language Assistance Preference Form also found on our website www.calchoice.com. www.calchoice.com ... |
|
Change Request Form
This form must be received by CaliforniaChoice no later than 60 days after the event takes place if outside E-mail to: memberprocessing@calchoice.com. |
|
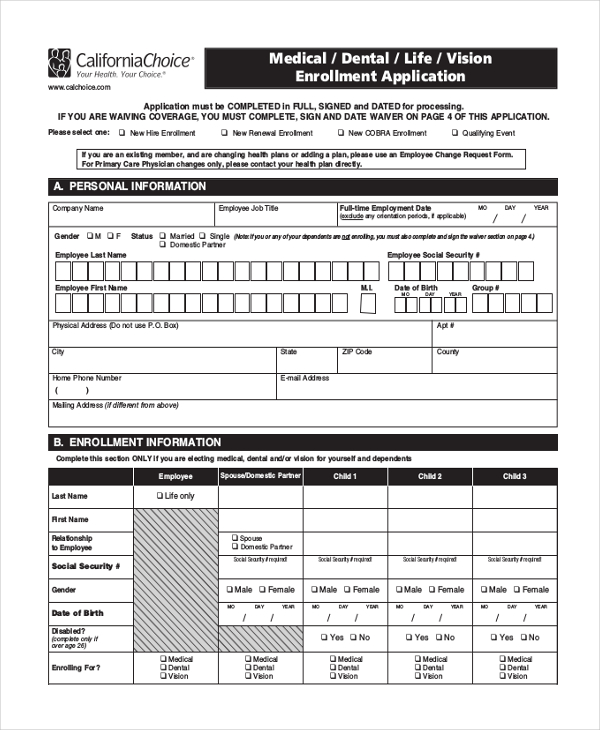
Medical / Dental / Life / Vision Enrollment Application
01-Sept-2019 COBRA. Cal-COBRA. PLEASE SIGN AND DATE APPLICABLE SECTIONS INSIDE ... COMPLETE AN EMPLOYEE CHANGE REQUEST FORM IF YOU ARE AN EXISTING MEMBER ... |
|
Medical / Dental / Life / Vision Enrollment Application
Cal-COBRA. PLEASE SIGN AND DATE APPLICABLE SECTIONS INSIDE APPLICATION. 721 South Parker Suite 200 |
|
EMPLOYER ADMINISTRATIVE GUIDE - CaliforniaChoice
Employer Responsibilities For Cal-COBRA Language Assistance Preference Form also found on our website www calchoice com www calchoice com |
|
COBRA/CalCOBRA Process (post termination)
Employee Termination Form Federal COBRA Participant A 2 admin fee is added if WageWorks is the COBRA administrator through CalChoice |
|
CC0208_Group_COBRA_Billing_Contact_92019 (4082 - Activated
(800) 558-8003 • www calchoice com Group COBRA Billing Contract regulations be sent directly to the group to be forwarded to the COBRA participants |
|
CalChoice - Sharp Health Plan
appropriate request form is submitted to the Employer within 45 days after PLAN has agreed to provide coverage for you if you are Cal-COBRA-eligible or |
|
CaliforniaChoice® Small Business
calchoice com COBRA Cal-COBRA Billing: Includes participant invoicing, premium collection and remittance, Owner/Partner form for owners/partners not |
|
UNDERWRITING GUIDELINES - CaliforniaChoice
calchoice com 800 542 4218 simple Cal-COBRA eligible) employees and enrolling dependents; Owner/Partner form for owners/partners not listed on the |
|
Medical / Dental / Life / Vision Enrollment Application - Dickerson
1 sept 2019 · COBRA Cal-COBRA PLEASE SIGN AND DATE APPLICABLE SECTIONS INSIDE APPLICATION COMPLETE AN EMPLOYEE CHANGE REQUEST FORM IF YOU ARE AN EXISTING (800) 558-8003 www calchoice com |
|
WageWorks COBRA Administration Guide
If one of your employees gets married and adds the new spouse to one of the COBRA eligible benefits, the spouse must be sent a DOL General Notice Send the |
|
CaliforniaChoice—Medical/Dental/Life/Vision Enrollment
CalChoice® HMO 25 Value This form must be completed and signed by the employee Failure to complete and an eligible COBRA/Cal-COBRA participant |